Case study: alopecia areata hair loss – its symptoms, treatment and recovery
04.04.23
Alopecia Areata (AA), is one of the most common hair loss conditions after androgentic alopecia (male or female pattern hair loss). Research suggests that 2 in every 100 people could be susceptible to AA worldwide, which is associated with mental health, anxiety and autoimmune conditions.[1]
In this case study we talk about the the onset of AA in one of our clients, Mary*, the treatment protocols we recommended and how the condition was managed.
Introducing Mary
Mary, age 25, contacted us for an initial consultation to discuss her concerns and anxiety over a sudden onset of what she described as “patchy hair loss“.
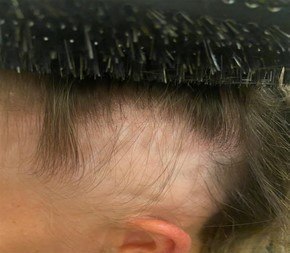
On the video, Mary presented with five circular patches of hair loss, varying in size from 1cm in diameter to 6cm in diameter.
Three larger circular patches, which were 3cm in diameter, were in the vertex/ crown region, the fourth patch was a large 5cm patch on the left-hand side above the ear, and the fifth patch was located on the front hairline; this was approximately 1 cm in diameter. Looking closely at the areas of hair loss during the video consultation, there was the appearance of very short ‘stubby’ broken hairs around the perimeter of each hair loss patch.
Mary’s presenting symptoms were typical associations of the Alopecia Areata (AA) condition.
The prognosis for AA is particularly unpredictable. Recent data states spontaneous regrowth can occur in a 35 – 50% of people in a 12-month time frame, while up to 25% of people may progress into Alopecia Totalis or Universalis.[2]
While AA is not curable, if less than 50% of the head is affected, then this is considered a mild case. This was the case for Mary. However, the emotional impacts of hair loss are often significant. Starting quick treatment for the condition can help improve the chances of a quicker recovery.
After discussing her diagnosis with Mary, we created a treatment pathway. We put this treatment into 3 categories: self-care, clinical care and medical care.
Self Care
For self-care we recommended Mary consider working with a professional to help her manage the anxiety, as stress is considered a possible exacerbater for AA.
We also recommended using our genetic test, which was applied at home, and this would provide a more detailed recommendation for supplements, vitamins and prescriptions.
We maintained our support with a follow-up consultation in twelve weeks to determine progress.
Clinical Care
For clinical care, we recommended Mary benefit from specialist treatment, intralesional steroid injections into the hair loss patch areas, which she received from a dermatologist who received our detailed consultation report.
Medical Care
The genetic test identified a personalised prescription of topical steroid and minoxidil 5% which was applied daily for several weeks.
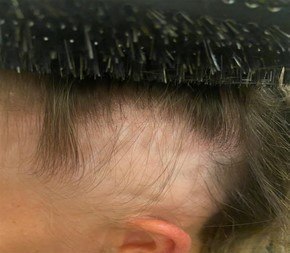
After three months of the treatment pathway, Mary’s hair was shown to have responded positively to the medications and treatment. The patch above the left ear had reduced in size by 2cm and the other four patches was almost completely recovered.
Here are images of the large patch of AA at the onset before the treatment and three months after the treatment plan.

The key insight into Mary’s story is not to wait or self-diagnose. This treatment plan worked after a successful diagnosis and using genetic testing. The holistic overview supporting her mental health, diet and treatments enabled a fairly quick response to a condition causing anxiety.
Book your initial video consultation HERE if you have a concern about hair loss and need an immediate diagnosis.
References:
1Miteva M, Villasante A. Epidemiology and burden of alopecia areata: a systematic review. CCID. Published online July 2015
2 Darwin E, Hirt P, Fertig R, Doliner B, Delcanto G, Jimenez J. Alopecia areata: Review of epidemiology, clinical features, pathogenesis, and new treatment options. International Journal of Trichology.
* name changed for anonymity
